How Baby Steps helps put new parents on a firm footing
Charlotte Goddard
Monday, July 29, 2019
NSPCC programme sees new parents who may be less likely to access antenatal education receive the support that can transform outcomes for their families.

PROJECT
Baby Steps
PURPOSE
To increase families' access to support services, childcare, and financial benefits, and improve parental wellbeing
FUNDING
Organisations delivering the programme pay a fee, covering training for 12 people, materials, and ongoing support for three years
BACKGROUND
Antenatal education focusing on the transition to parenthood, the relationship between partners, and the development of positive bonds between babies and parents, can improve outcomes for both parents and children. The NSPCC worked with Warwick University to develop Baby Steps for new parents more likely to need extra help and less likely to access antenatal education.
"We did some scoping work around perinatal education and vulnerable families and it showed gaps in provision," says Victoria Joel, implementation manager at the charity. "The most vulnerable do not attend antenatal care."
Organisations and local authorities can sign up to deliver the programme and the NSPCC also delivers it directly in some areas. In some places, such as Blackpool and Jersey, Baby Steps is being offered as a universal antenatal programme while other areas such as Warwickshire, Wiltshire and Swindon are running it as a targeted scheme.
ACTION
Baby Steps is co-delivered by a children's services professional, often a family support worker, alongside a healthcare professional such as a midwife or health visitor. "We think this provides parents with a more holistic approach," says Joel. "Vulnerable families have a lot of needs so it is useful to have a social worker involved."
The NSPCC supports external sites to set up the programme. Practitioners receive training before delivering the groups and again four to six months into the programme. "We provide ongoing support including practice days twice a year, reflective training for managers and a yearly review so organisations can share where they think they are at and if anything needs to be improved," says Joel. While many aspects of the programme are fixed, some elements can be adapted to meet local needs.
Parents-to-be may self-refer or may be referred by professionals including social workers, health visitors, midwives and GPs. Those taking part in the groups could be facing a range of issues including drug or alcohol problems, difficulty reading, speaking or understanding English, low-level mental health problems and homelessness. Participants receive a home visit in the seventh month of pregnancy and then attend six weekly group sessions before the baby is born.
"The initial home visit is to encourage attendance," says Joel. "Having them see your face really helps, and you can pick up what might affect their ability to attend such as concerns about bus routes, or a disinclination to speak in groups."
The sessions are interactive and include films, group discussions and creative activities designed to build confidence, communication skills and relationships between parents and their babies. The six sessions cover the development of the unborn baby, how a new child is likely to impact on parents' lives, the health and wellbeing of parents, giving birth, caring for the baby, and the support services available.
"We are trying to increase the parents' bond with the baby, so we might have an activity where mum and dad write some of the characteristics they hope the baby might have," explains Joel. "When the baby is born they can see if their predictions are right. It gets parents thinking about the unborn child as a real person."
After the birth the family is visited again at home, and then attends a further three group sessions with the babies. "The second home visit is to re-engage the family and to show you have been thinking of them," says Joel. The facilitator records a short video, showing positive moments between the parents and the baby. When the group restarts parents view the footage with the facilitators so they can see how their baby is responding to their actions. "Then the footage is given to them, maybe on DVD or as a picture," says Joel. "Some parents have told me they put the photo on the fridge to remind themselves they are a good parent during difficult days." During these postnatal groups the facilitators will flag up further community services, such as baby massage or toddler groups.
OUTCOME
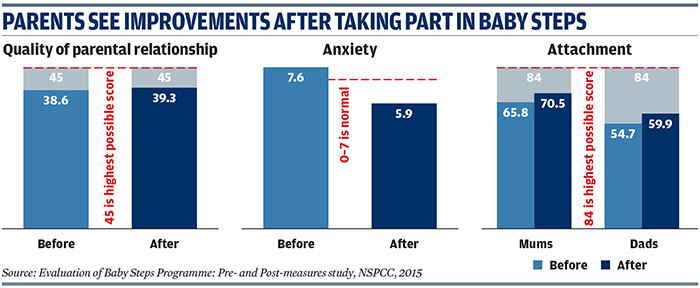
An NSPCC evaluation published in 2015 found parents rated the quality of their relationship more highly after the antenatal sessions, with average scores rising from 38.6 to 39.3 on the Relationship Quality Index where the highest possible score is 45. On average, participants' self-esteem rose following the programme, from an average of 19.8 on the Rosenberg Self Esteem Scale to an average of 22.5. A score of 15 to 25 is considered normal. Anxiety levels fell, from 7.6 to 5.9 on the Hospital Anxiety and Depression Scale with scores between zero and seven considered normal.
Parents' attachment to their unborn baby rose between the first home visit and just before the birth. Before the programme mothers scored on average 65.8 and fathers 54.7 but after the antenatal sessions this rose to 70.5 and 59.9. The highest possible score is 84. Parents also showed improvements in their relationship with their baby after the birth. Average scores on the 35-point Mothers' Object Relations Scale, which measures mothers' perceptions of their baby's feelings towards them, increased from 21.16 to 28.18.
WHAT NEXT?
The NSPCC had begun to move away from running Baby Steps directly, focusing on supporting other organisations to deliver the programme. However, the charity now plans to step up its own delivery of the programme at the same time as supporting others "We are about to start again because having internal sites running it helps us if we want to do some qualitative learning or trial new things," says Joel. Baby Steps can help mothers-to-be who are at risk of antenatal depression
Baby Steps can help mothers-to-be who are at risk of antenatal depression
EXPERIENCE
Building a mother's confidence while reducing her anxiety
South Warwickshire NHS Foundation Trust runs the Baby Steps programme in Nuneaton and Bedworth, and launched it in Rugby this March.
Ashley* was referred to Baby Steps by her midwife because of her high levels of anxiety. At the time she was not with the baby's father so she attended the group at her local children's centre on her own, explains Caroline Baugh family nurse and baby steps co-ordinator at South Warwickshire. "Ashley said she felt the programme might be like school and that she found it hard to come into a group situation," says Baugh. "We felt she might be at risk of antenatal depression." With the support of the facilitators, Ashley spoke to her health visitor about a possible referral to the perinatal team and went to see her GP.
By the fourth week of the programme, Ashley was a lot calmer, says Baugh. "She said she enjoyed coming to the group, she met a few people." Ashley's difficult relationship with her mother was eased after her mum attended the group with her daughter.
After six weeks Ashley's evaluation showed her depression and anxiety levels were much lower. "Ashley told me ‘I feel so much more confident about things, I am looking forward to having my baby now'," says Baugh. "She and the baby's father decided to give their relationship another go, and he attended the last group." Talk and Listen Time was particularly helpful. "At the end of a session one person talks and the other listens. It gives one person a chance to talk, rather than both shouting." Ashley told Baugh her confidence had soared since attending the group.
"When I visited Ashley after the birth she was doing very well," says Baugh. "Breastfeeding was going well and she was very calm with the baby, showing great attachment."
*Name changed
If you think your project is worthy of inclusion, email supporting data to derren.hayes@markallengroup.com